MRI vs. Musculoskeletal Ultrasound: What Your MRI Isn’t Telling You
When it comes to using imaging to diagnose your pain, bigger is always better . . . right? According to that logic, an MRI—with its bulky equipment, lengthy scan time, and sizeable price tag—is your best bet for receiving the most comprehensive answers about your health. However, MRIs have their limitations, and, especially in the field of musculoskeletal injuries and conditions, may not be giving you the whole picture. Keep reading to discover three things your MRI is not telling you, and how a musculoskeletal ultrasound may be able to fill in the blanks.
But first, let’s identify the basic differences between MRI and ultrasound technology:
Magnetic resonance imaging (MRI) scanners use radio waves and powerful magnets to align water cells in the body in such a way that a computer can produce an image of both hard and soft tissue and organs. Although MRIs do not use radiation, due to the magnets, they are contraindicated for patients with metal embedded in their bodies.
Ultrasound (or sonography) sends high-frequency sound waves through a transducer (applied directly to the body) and the returning echo is captured by the transducer and translated into an image by the computer. Ultrasounds also do not use radiation and are less physically restrictive for patients.
Now, let’s get back to our discussion of MRIs and ultrasounds, which has been divided into three categories here: movement, timing and totality.
Movement: How movement is affecting your pain and diagnosis
Have you ever had recurrent pain in a joint that only manifested when you were actually using it? Like going to the doctor for a persistent cough only to have the cough disappear two minutes before the doctor comes in, having pain that is only present in certain conditions can be frustrating to properly diagnose and treat if those conditions can’t be replicated. MRI is considered a static imaging technique, meaning it is a still image. In fact, patient movement during an MRI may invalidate the findings. An ultrasound, however, can capture movement as it is happening. This can help your doctor understand if the pain is caused by the movement itself or by another issue, which may be invaluable for determining a correct diagnosis.
Timing: What your injury looks like at the time of your examination or procedure
Although an MRI is a powerful tool, it is also a snapshot of your body. As with any type of snapshot, the moment an image is captured, it starts to become outdated: our bodies continue to age and change with every minute that goes by (whether we like it or not). Logistically, it’s not practical to have MRI machines in exam rooms to be used at a moment’s notice or for care providers to be scanning while simultaneously administering injections. However, when performing in-office procedures or targeted treatments, bedside imaging is incredibly useful. Rather than providers working from dated images and using anatomic landmarks to locate approximate treatment points, ultrasound imaging allows them to ascertain the most current state of the injuries being treated and can guide providers in delivering the most accurate subdermal treatments.
Totality: The whole picture of your condition
So, can bigger ever be better when it comes to imaging? In many cases, the answer will be, yes. However, due to the nature of the large MRI scanners and how they capture images, musculoskeletal ultrasounds have actually been found to be more effective at capturing the entire length of longer structures like tendons, nerves and muscles. The ultrasounds’ agile transducer can also be maneuvered into more awkward angles to capture views that the larger scanners cannot, giving your provider even more insight into your condition.
At the end of the day, ultrasounds are not here to completely replace MRIs. In fact, ultrasounds can’t penetrate bone and they can’t accurately visualize gas- or air-filled organs such as the lungs or bowels. But when it comes to understanding and capturing aches and pains related to the musculoskeletal system, ultrasounds are uniquely suited to the task, not to mention they are more affordable, more convenient and more comfortable for patients.
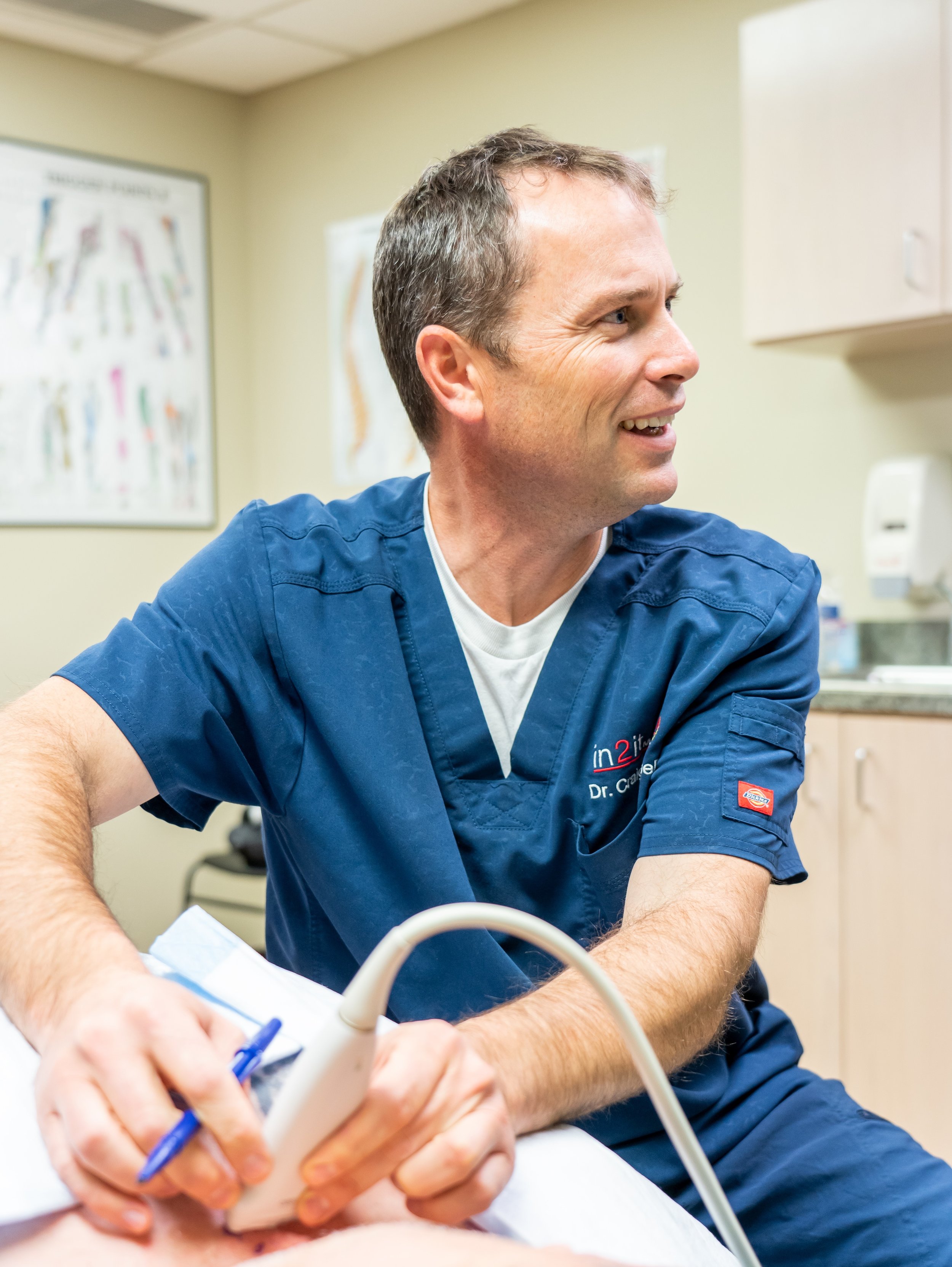
Want to see a musculoskeletal ultrasound in action? Click here to watch Dr. Chappell demonstrate an ultrasound’s ability to capture movement and guide a procedure.
Sources
Peck J, Gustafson KE, Bahner DP. Diagnosis of Achilles tendon rupture with ultrasound in the emergency department setting. Int J Acad Med [serial online] 2017 [cited 2019 Jan 30];3, Suppl S1:205-7. Available from: http://www.ijam-web.org/text.asp?2017/3/3/205/204947
https://www.radiologyinfo.org/en/info.cfm?pg=musculous
https://www.radiologyinfo.org/en/info.cfm?pg=muscmr